Hips and a New Workout Regimen
/Before jumping into what amounted to a fairly important two days in my training and tri-writing career, I wanted to share my second "Mind Games" column for Lava Magazine online. I'm pretty proud of this one, and hope it somehow helps you in your training if you've ever gone through or are going through some tough times right now. If you haven't already, check it out and let me know what ya think or if you've found other methods have helped you overcome disappointment. OK, now to our regularly scheduled blog post. Apologies for not writing last night -- Steph and I had a wedding-related class and got home late.
So here below is an unedited IM chat my physical trainer, Shannan, shared with me that she had with a grad school professor of hers. He’s a Ph.D. in biomechanics and doctor of physical therapy. This conversation occurred after I described to Shannan my ART therapist's analysis of my hip area problems, which were initially diagnosed as psoas-related, then we moved to the hip flexor, and now we've been looking at the gluteus medius. This of course relates to all the post IM Arizona problems I've been having.
Shannan thought the problem may be something else. And she's been right about me before. Shannan's the one who attributed my early IT band troubles in my running career to flat feet and advised I get fitted with orthotics. I did, and my IT band problems went away. So, Shannan has accurately predicted things in the past.
Here's the IM chat:
Shannan: Hey- I have a case study for you, 90% sure it’s trochanteric bursitis or G. medius tendonitis; abnormal hip pathology is primary symptom.
Male; mid-30’s; fine-boned; ironman finisher; significant pronator (wears bilateral orthotics); confirmed leg-length discrepancy; palpable abnormality at the greater trochanter. His ART guy thinks it’s an overactive G.med but unless he strained it there’s no way…I can visually see a mass and I can feel the difference.
Doctor: History of back injury? Lower back problems, glute insufficiencies? What are his running habits (trail, road, treadmill)?
Shannan: He has spondy, little scoliosis, glutes are pretty insufficient but no L4-S1 acute injuries that I know about; in other words nothing that would prevent building them up. He does a lot of trail running…
Doctor: I would do a Trendelenburg test to check out his abductor reflexes.
Shannan: Yeah, I’m thinking it’s an abductor weakness (not overworked as the ART therapist suggested), but I stopped the abductor exercises because I don’t want to provoke the inflammation??
Doctor: Right, usually an ultrasound is needed to determine exact etiology; however, bursitis will not cause pain upon resisted abduction, but G. medius will hurt like a mo fo (well, mo fo point tenderness pain). Keep off the abductor exercises until pain goes away a bit, but you’re correct in diagnosing the abd weakness. Build up his glutes, too.
Shannan: What about stretching? Deep tiss massage?
Doctor: Massage is good to deliver blood flow; stretch all he wants, but it’s not going to help if it’s articular. I suggest he gets those orthotics checked; at the rate he trains he may need a new set every 6 months. Also, until the condition improves I do not recommend trail running because the uneven surface does not help- both conditions are caused by some type of asymmetry, and trail running is contradictory. I understand the training demands, but he should run on flat surfaces. ART is fine, never hurts. What’s his size?
Shannan: He’s 5’7” and probably around 137-140 this week. Fine-boned
Doctor: He’ll have a double hip replacement at this rate…
Aside from being mildly annoyed with being called "fine-boned" (what am I, a herring?), the last sentence obviously got my attention. It's what occupied a good portion of discussion today in my personal training session with Shannan. Fortunately, she doesn't think I'm on track for such a dreadful fate. It was the doctor being off-the-cuff and dramatic, in her words.
Instead, after doing some mobility drills and balance tests where I stood on one-leg and resisted pressure using my legs to push outward, Shannan thinks the problem is tendinitis or bursitis in the hip joint that connects the femur. That would explain the puffiness as it's likely fluid build-up. The solution, in her opinion, is getting an ultrasound at my MD office and then a shot to reduce the inflammation.
That sounds a LOT better than replacing two bad hips!
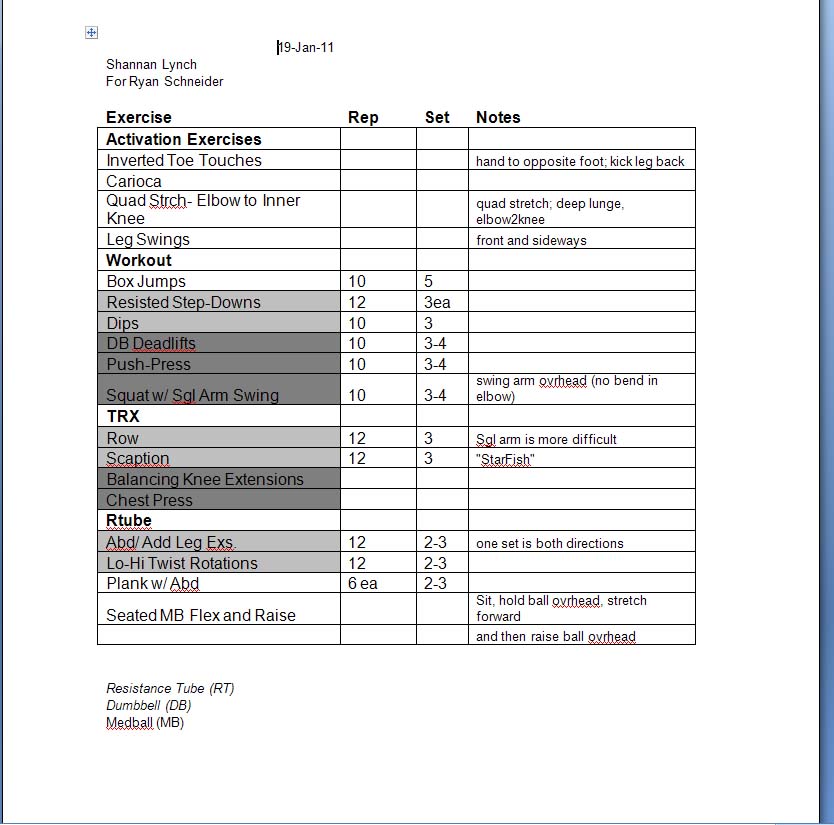
To combat the problem, Shannan produced the following workout regimen. I'll be doing this twice a week for the next few weeks and will let you know how it goes.
153 days and counting.
PS: I have contacted Newton about reviewing a pair of shoes for the blog based on your passionate feedback about how much good they've done some of you. So far, Newton has been amazingly responsive and open. I'm embarking upon this experiment against the wishes of my coach and ART therapist. But that's where the potential lies for a great story. I'm thinking of it as the Newton Challenge. If they're good for me, they're good for anyone. Newton's up for the challenge and I'm up for the risk. I'll use the shoes exactly as intended in the ramp-up period and share what I find at the end. I'll drop a few snippets here on the blog to give you an idea on how it's going.